Common Signs of Peritoneal Mesothelioma
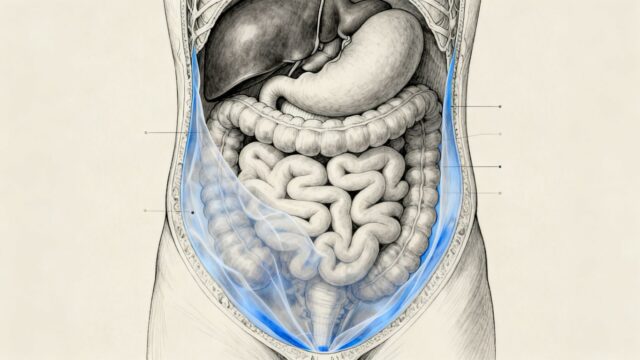
Peritoneal mesothelioma, a rare cancer affecting the lining of the abdomen, often develops slowly over many years. Because it originates in the peritoneum, the symptoms can be quite varied and sometimes mimic less serious conditions. Many individuals are diagnosed in their 50s or later. The most frequently reported signs include a general sense of abdominal pain that might feel spread out, or a noticeable swelling or bulging of the abdomen. This swelling is often due to a buildup of fluid, a condition known as ascites. Changes in bowel habits, such as constipation or even a bowel obstruction, can also occur. Other common indicators might include nausea, vomiting, and a general loss of appetite. It’s important to note that these symptoms can be subtle and may not be immediately recognized as signs of a serious illness.
Subtle Early Symptoms
In its initial stages, peritoneal mesothelioma might present with very mild or easily overlooked symptoms. Sometimes, the first indication is simply an unexplained increase in abdominal girth, making clothes feel tighter or causing a visible change in the abdominal profile. Some individuals might experience a persistent, dull ache in the abdomen that doesn’t seem to resolve. Others might notice a new hernia, which can be a sign of increased pressure within the abdominal cavity. Less commonly, early signs could include a low-grade fever or night sweats, or a general feeling of fatigue and weakness. These early, subtle signs are often attributed to other causes, delaying a proper diagnosis.
Symptoms Indicating Advanced Disease
As peritoneal mesothelioma progresses, the symptoms tend to become more pronounced and severe. Significant abdominal pain and a distended abdomen due to substantial fluid accumulation (ascites) are common. Patients may experience significant weight loss and a noticeable decrease in appetite. In advanced stages, complications can arise, such as a complete bowel obstruction, which is a medical emergency requiring immediate attention. Other severe symptoms might include vomiting, persistent fever, and the development of a palpable mass in the abdominal or pelvic area. In some rare instances, advanced disease can lead to paraneoplastic syndromes, which are conditions triggered by the cancer that affect other parts of the body, such as blood clotting disorders or severe fatigue.
The Diagnostic Process for Peritoneal Mesothelioma
Diagnosing peritoneal mesothelioma can be a complex process, often involving a series of tests to confirm the presence of the cancer and determine its extent. Because the symptoms can be vague and mimic other common ailments, it’s not unusual for the disease to be identified at later stages.
Initial Evaluation and Physical Examination
The diagnostic journey typically begins with a thorough medical history and a physical examination. Your doctor will ask about your symptoms, any history of asbestos exposure, and other relevant factors. During the physical exam, the physician will carefully palpate your abdomen to check for any unusual masses, swelling, or tenderness. This initial assessment helps guide the subsequent diagnostic steps.
Role of Imaging and Blood Tests
Following the initial evaluation, various imaging techniques and blood tests may be ordered. Imaging scans such as CT (computed tomography), MRI (magnetic resonance imaging), and PET (positron emission tomography) scans can help visualize the abdominal cavity, identify any tumors, and assess their size and spread. These scans can reveal abnormalities like ascites (fluid buildup in the abdomen) or omental caking (thickening of the abdominal lining). Blood tests may be conducted to look for specific biomarkers, such as CA-125 or mesothelin, which can sometimes be elevated in individuals with mesothelioma. However, it’s important to note that these markers are not exclusive to mesothelioma and can be present in other conditions as well. The findings from these tests, while suggestive, are not definitive for a diagnosis. For instance, CT scans might show signs typical of many abdominal cancers, making it difficult to pinpoint peritoneal mesothelioma without further investigation. This is why further steps are usually necessary to confirm the diagnosis.
The Definitive Role of Biopsy
Ultimately, a definitive diagnosis of peritoneal mesothelioma relies on a biopsy, and understanding what the peritoneal mesothelioma diagnostic process involves can help patients prepare for what lies ahead. This procedure involves obtaining a small sample of tissue or fluid from the affected area. The sample is then examined under a microscope by a pathologist, who can identify the characteristic cells of mesothelioma. There are a few ways a biopsy can be performed. Sometimes, a minimally invasive procedure called laparoscopy is used, where a small incision is made to insert a camera and instruments. In other cases, a larger surgical procedure might be necessary to obtain adequate tissue samples. The pathologist will also use special stains and sometimes electron microscopy to distinguish mesothelioma from other types of abdominal cancers, such as ovarian or colorectal cancer. A biopsy remains the gold standard for confirming peritoneal mesothelioma.
Distinguishing Peritoneal Mesothelioma from Other Conditions
Similarities with Other Peritoneal Cancers
Peritoneal mesothelioma can present with symptoms that overlap significantly with other cancers affecting the abdominal lining. This similarity often makes initial diagnosis challenging. Conditions like pseudomyxoma peritonei, which originates from the appendix, as well as ovarian, colorectal, and other peritoneal sarcomas, can mimic peritoneal mesothelioma. These cancers often lead to similar issues such as abdominal pain, swelling, and changes in bowel habits. The non-specific nature of these symptoms means that patients may not seek medical attention until the disease has progressed considerably.
Challenges in Differentiating Symptoms
The symptoms of peritoneal mesothelioma are frequently vague and can be easily mistaken for less serious gastrointestinal issues. This can lead to delays in diagnosis. Common signs include abdominal discomfort, a feeling of fullness, nausea, and unexplained weight loss. In more advanced stages, patients might experience significant fluid buildup in the abdomen (ascites), bowel obstruction, or even a hernia. These symptoms are not unique to mesothelioma and can be present in a wide range of abdominal conditions, making it difficult to pinpoint the exact cause without further investigation.
Importance of Medical History and Exposure
Given the overlapping symptoms, a thorough medical history is absolutely vital in the diagnostic process. This includes understanding a patient’s past occupational and environmental exposures. While asbestos exposure is a well-known risk factor for pleural mesothelioma, its association with peritoneal mesothelioma is less pronounced, accounting for about 30% to 40% of cases. This means that for a significant number of patients, the cause remains unknown. However, any history of asbestos exposure, even from decades prior, should be carefully considered. Additionally, understanding the patient’s overall health and any pre-existing conditions helps physicians rule out other potential causes and narrow down the possibilities. This careful evaluation is key to distinguishing peritoneal mesothelioma from other abdominal cancers and conditions, guiding the path toward accurate diagnosis and appropriate treatment Malignant pleural mesothelioma.
Treatment Modalities for Peritoneal Mesothelioma
Surgical Interventions
When it comes to treating peritoneal mesothelioma, surgery often plays a significant role, particularly in removing as much of the cancerous tissue as possible. This procedure, known as cytoreductive surgery, aims to debulk the tumors. It’s frequently followed by a process called hyperthermic intraperitoneal chemotherapy, or HIPEC. During HIPEC, heated chemotherapy drugs are circulated directly within the abdominal cavity. This two-step approach is considered a primary treatment for many patients with this condition.
Chemotherapy and HIPEC
Chemotherapy remains a cornerstone in managing peritoneal mesothelioma. Beyond its use during surgery with HIPEC, systemic chemotherapy drugs are administered to target and destroy cancer cells throughout the body. These medications can be given before or after surgery, or as a standalone treatment if surgery isn’t an option. The specific drugs and combinations used are tailored to the individual patient’s situation. For instance, combinations like cisplatin and pemetrexed have been studied, though survival benefits from systemic chemotherapy alone are often modest, typically around a year. HIPEC, however, offers more promising outcomes when combined with cytoreductive surgery, with some studies showing significant long-term survival rates for eligible patients.
Emerging Therapies and Palliative Care
While surgery and chemotherapy are established treatments, research continues to explore new avenues for patients whose diagnosed peritoneal mesothelioma has progressed beyond what conventional approaches can address. Immunotherapy, which harnesses the body’s own immune system to fight cancer, is one such area. Targeted therapies are also being investigated, focusing on specific genetic alterations within cancer cells. These approaches may be used alone or in combination with traditional methods. For patients whose disease is more advanced or who are not candidates for aggressive treatment, palliative care becomes important. This focuses on managing symptoms, improving quality of life, and providing support throughout the illness, rather than solely aiming for a cure. Clinical trials are also an option for patients seeking access to novel treatments.
Risk Factors and Causes of Peritoneal Mesothelioma
Peritoneal mesothelioma is a challenging disease, and there’s still a lot scientists don’t completely know about why it develops in some people and not in others. One thing researchers agree on is that a few factors really do increase the odds. Let’s break down what’s known about the causes and risk factors behind this cancer.
The Role of Asbestos Exposure
Asbestos is pretty much the prime suspect when it comes to the cause of peritoneal mesothelioma. Most people who get this disease have a history of coming into contact with asbestos at work or in the environment, even if it was decades earlier. Asbestos fibers can get lodged in the peritoneum (the lining of the abdomen) and sit there for years before triggering cancer.
There are three ways exposure might happen:
- Direct occupational exposure: Jobs in construction, plumbing, shipyards, and manufacturing have put people in contact with asbestos.
- Secondary exposure: Family members can come into contact with asbestos fibers brought home on work clothes, hair, or even skin. Everyday tasks like laundry have been a source of risk, as described by studies on occupational and secondary asbestos exposure.
- Environmental exposure: Living near asbestos mines or factories can increase risk even if you never work with the material yourself.
The amount and length of exposure matter—a little contact sometimes is enough, but longer or repeated exposures raise the risk a lot, a pattern consistent with mesothelioma diagnosis patterns seen across occupational exposure cases.
Other Potential Contributing Factors
Sure, asbestos is the big one, but it’s not the only thing to keep in mind. A few other possible contributors include:
- Age: It’s more common in people over 50, since the disease takes years to develop after exposure.
- Radiation: Rarely, radiation to the abdomen for other cancers has played a role.
- Mineral exposure: Some minerals like silica or erionite, found in certain geographic locations, have a similar effect as asbestos in rare instances.
- Talc contamination: There have been cases where the use of talcum powder contaminated with asbestos has increased risk, especially among women.
- Household products: Though less common now, some old insulation and fireproofing materials can expose users to asbestos.
Genetic Predispositions
There’s some evidence that people who have inherited specific gene mutations might be more likely to develop peritoneal mesothelioma if they’re exposed to asbestos. For example, mutations in the BAP1 gene can increase risk. This gene is involved in repairing damaged DNA, so if something goes wrong with it, cells can be more likely to turn cancerous.
Family history seems to play a role too, although exactly how isn’t fully understood. It could be genetics, a shared environment, or both. The bottom line? Most people who get peritoneal mesothelioma have at least one risk factor, usually some form of asbestos exposure, but it’s possible for the disease to show up even in people with no clear cause.
Prognosis and Life Expectancy
Factors Influencing Prognosis
Understanding what shapes prognosis for peritoneal mesothelioma can help patients and families manage expectations. No two patients will have the exact same journey, so it’s important to look at the big picture. Here are some factors that often influence the outcome:
- Stage of the disease at the time it’s found
- The patient’s age and overall health
- Type of mesothelioma cells (cell subtype)
- Whether the patient can undergo surgery
- Gender and genetics may also have a role
Some people live far longer than average, but most statistics focus on large groups, not individuals. Women sometimes have a slightly better outlook than men, and dedicated resources on mesothelioma in women explore the unique exposure histories, diagnostic challenges, and treatment considerations that affect this group.
Impact of Treatment on Survival
Choice of treatment can really change the outlook. For those who receive both surgery and heated chemotherapy (HIPEC), some studies say average survival can reach around 31 months after diagnosis. If patients can’t have surgery and get only chemotherapy, the average is closer to 13 months. When no treatment is possible, it’s much shorter—usually 6 to 8 months. Usually, people treated for peritoneal mesothelioma can expect to live between 12 and 21 months.
A few outliers have lived far beyond these averages, especially when the disease is caught early. Trying new or experimental therapies may also extend life, and quality of life is sometimes as important as length.
Living With Peritoneal Mesothelioma
Getting a diagnosis of peritoneal mesothelioma changes many parts of daily life. People face emotional stress, changes in eating or sleeping habits, and worries about the future. Support from loved ones and regular visits to care teams become more important.
A few tips for living with this disease:
- Keep open communication with doctors and nurses
- Join a support group, even if just online
- Take manageable steps to maintain strength and mood
Some patients find meaning or new perspective from their experiences. Quality time with friends and family, enjoying small pleasures, or even an ordinary walk can take on new importance. It becomes about more than survival; it’s about finding moments of comfort and joy, even in difficult times.