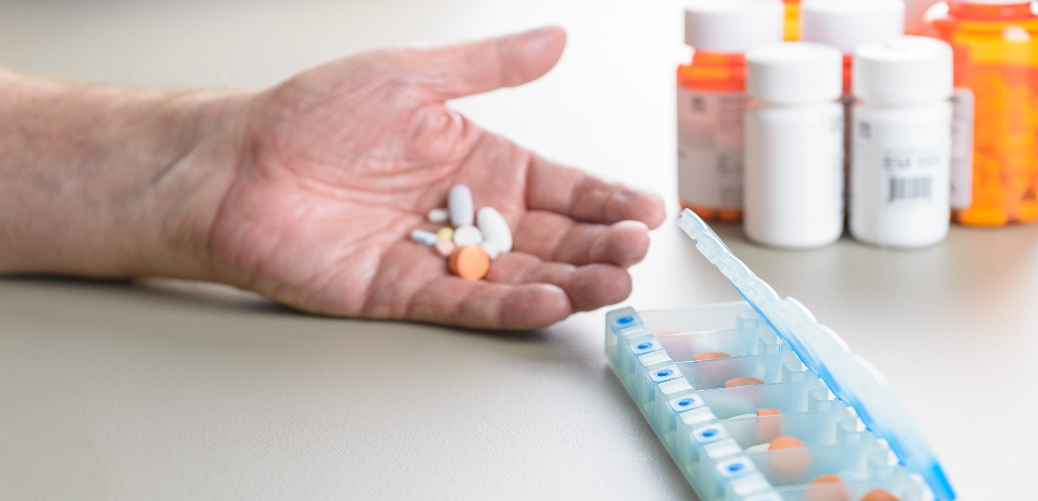
In literal terms, polypharmacy means “multiple medicines”. It refers to a patient taking a number of different medications concurrently, either over the counter or prescription.
When it comes to “how much is too much” there’s no specific rule. Some medical professionals would class polypharmacy as taking only two medications at once, whereas others would allow up to 20. Usually however, around five medications taken at once would be accepted as polypharmacy.
Who is most vulnerable to polypharmacy?
Elderly patients are most susceptible to polypharmacy as well as those with chronic physical and/or mental health conditions. It is thought that around 20% of adults with intellectual disabilities are at risk of expose to polypharmacy.
What are the dangers?
Polypharmacy is of great concern in older patients as they are deemed to be at higher risk of adverse drug reactions (ADRs). This is because age often causes metabolism to slow, so medications taken by older people are typically absorbed less quickly. The more drugs that are used, the worse this can be.
Another factor is accidental overdose. Patients suffering from dementia or general cognitive decline may well forget which medications they’ve already taken and when, leading to double dosing. Finally, drug interactions can bring about a range of unpleasant side effects that will require management and potentially treatment.
Signs and symptoms
There are a number of possible symptoms of polypharmacy. They include:
- Confusion
- Falls
- Dizziness
- Loss of appetite
- Weakness
- Depression
- Anxiety
- Tiredness or decreased alertness
- Tremors
Managing polypharmacy
Achieving the best outcomes for patients can only happen when polypharmacy is managed properly. Gaining a balance is essential, as under-prescribing is likely to be as harmful as over-prescribing. This makes it so important to provide patients with a clear plan of care alongside regular medication assessment.
Are you concerned about the risks of polypharmacy?
You may well find PDUK’s online course useful: My patient is on too many medicines. What do I do?
Ideal for all disciplines of nursing, the course looks at polypharmacy and structured medication reviews in detail. Held entirely online it’s perfect for socially distanced learning from home and is worth 4 hours of CPD over half a day. It also provides participants with a chance to use different tools that can be applied when working with patients at risk of polypharmacy issues.
The next session is planned for the 30th April 2021, so book your place today.
And while you’re there…
Our Medicines optimisation in Hypertension and Heart Failure is also well worth considering.
Again offered remotely, the course looks specifically at pharmaceutical management of patients with hypertension and cardiac failure. It also explores important issues faced by non-medical prescribers including patient monitoring and polypharmacy. Structured medication reviews will be discussed too, along with current guidelines.
The perfect course for anyone wishing to keep their skills up to date, it’s aimed at nurses and allied health professionals looking to broaden their knowledge in an interactive setting.
Also worth 4 hours of CPD over half a day. For course dates, check out the Practitioner Development UK website. Medicines optimisation in Hypertension and Heart Failure